Piriformis
- Fysiobasen

- Apr 17
- 8 min read
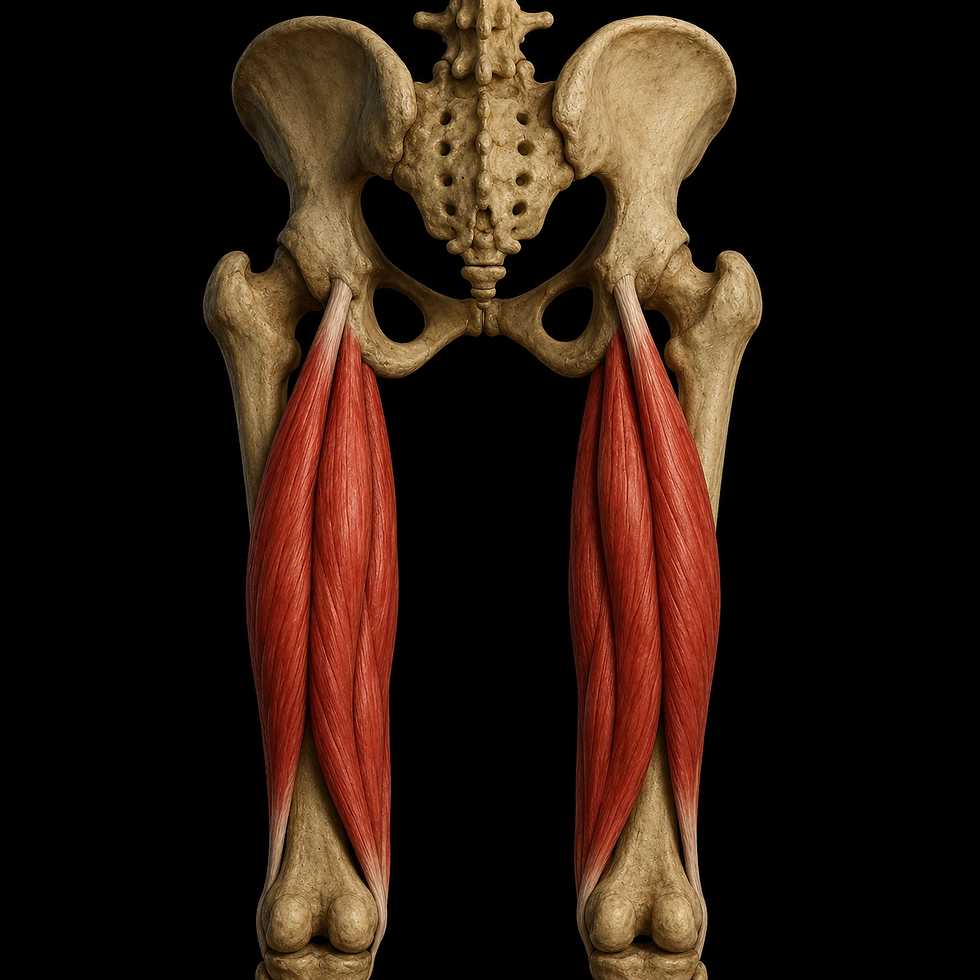
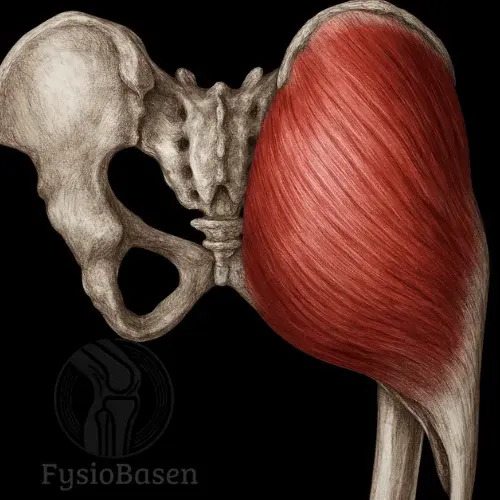
Piriformis is a thick, flat, and triangular muscle located deep in the gluteal region, but it is the most superficial of the deep lateral rotators of the hip. Its shape resembles a pear seed, which is where the name piriformis comes from, from the Latin piri (pear) and formis (shaped like). The muscle belongs to a functional group of six small but important muscles specialized in external rotation and stabilization of the hip joint. The others are obturator internus and externus, gemellus superior and inferior, as well as quadratus femoris¹.

Piriformis is particularly interesting clinically because in many cases it has a close anatomical relationship with the sciatic nerve, which passes just below the muscle, or in some individuals through or above it, as it leaves the pelvis through the greater sciatic foramen. This means that piriformis is both an important landmark for orientation in the gluteal region and a potential cause of sciatica-like pain, known as piriformis syndrome².
Origin and Insertion
Piriformis originates from the anterior surface of the sacrum, between the second and fourth sacral foramina, S2–S4, and to a lesser extent from the sacrotuberous ligament and the margin of the greater sciatic foramen. From there, the muscle runs laterally and leaves the pelvis through the greater sciatic foramen. It then inserts onto the superior and medial aspect of the greater trochanter of the femur³.
The muscle therefore travels from a medial and ventral position in the pelvis to a lateral and dorsal position in the gluteal region, forming a distinct diagonal line beneath gluteus maximus. Its location makes it relatively easy to identify in cross-section and during palpation against the sacrum.
Innervation and Blood Supply
Piriformis is innervated by its own nerve, called the nerve to piriformis, which is formed by anterior branches from S1 and S2⁴. It is therefore not part of the common nerve roots of the lower extremity, but rather a specialized branch of the sacral plexus.
The blood supply comes from several branches of the internal iliac artery, including:
• Superior gluteal artery
• Inferior gluteal artery
• Internal pudendal artery⁵
This composite blood supply is due to the muscle’s position as a transition zone between the vascular supply of the pelvis and that of the gluteal region.
Relationship to Other Structures
Piriformis functions as an anatomical dividing line in the gluteal region. Anything located above the muscle is referred to as suprapiriform, and anything below it as infrapiriform.
This division applies to:
• Nerves, for example the superior gluteal nerve above, and the sciatic nerve and inferior gluteal nerve below
• Arteries, with corresponding names and courses⁶
It is precisely because the sciatic nerve passes below piriformis in most people that a tight or irritated muscle can compress the nerve and cause radiating pain in the leg, which is a central feature of piriformis syndrome.
Function of Piriformis
Piriformis is an important dynamic stabilizer of the hip joint, with several roles that depend on the position of the hip joint. Its main functions involve external rotation, abduction, and stabilization of the femur within the acetabulum, and it contributes during both static and dynamic movements. What makes piriformis especially interesting is that its function changes depending on the angle of the hip joint, especially whether the hip is flexed or not¹.
Primary Functions at the Hip Joint
When the hip joint is in neutral or extension, piriformis primarily functions as:
• An external rotator of the femur
• A stabilizer of the hip joint by keeping the femoral head centered in the acetabulum
• A slight posterior tilter of the pelvis through its pull on the sacrum
When the hip joint is flexed beyond 60–90 degrees, the vector of the muscle fibers changes in relation to the axis of rotation of the joint. In that case, piriformis functions as:
• An abductor of the thigh
• A contributor to internal rotation, although weakly and with some debate²
This shift in function occurs because the muscle rotates around the hip joint and changes its line of pull in flexion, which is an example of how muscles can have different functions depending on joint position.
Functional Role During Movement
Piriformis is activated during a variety of movements and contributes especially in the following situations:
• Walking: Stabilizes the hip joint during the stance phase and controls rotational movement during push-off
• Single-leg stance: Works together with gluteus medius and minimus to maintain pelvic stability
• Stair climbing and lunges: Acts as a stabilizer to prevent medial collapse at the hip and knee
• Rotational movements and sports requiring rotation: Provides precise control of the hip joint during rapid changes of direction³
Cooperation with Other Muscles
Piriformis is one of the six deep lateral rotators of the hip:
• Obturator internus
• Obturator externus
• Gemellus superior
• Gemellus inferior
• Quadratus femoris
Together, these muscles form a muscular “cap” around the dorsal side of the hip joint that:
• Counteracts unwanted medial rotation
• Strengthens the passive stability of the hip joint
• Works together with gluteus maximus in extension movements
In addition, piriformis interacts with gluteus medius and minimus to balance rotational forces in the frontal plane, and with iliopsoas and the adductor group as antagonistic and synergistic partners.
Piriformis and Pelvic Control
Piriformis also has an indirect role in pelvic control, particularly through its origin on the sacrum and its connection to the sacrotuberous ligament. This allows it to contribute to:
• Stabilization of the sacroiliac joint
• Transfer of force between the lower extremity and the trunk
• Regulation of sacral tilting during asymmetrical loading
This is important in many functional movements that require controlled weight transfer, for example walking on uneven terrain or carrying load on one leg.
Clinical Relevance in Movement Chains
Piriformis can easily become overactive or compensatory if:
• Gluteus medius or minimus are weak
• Lumbopelvic control is poor
• The adductors are shortened
Overactivity can lead to myofascial pain or pressure on the sciatic nerve, which forms the basis of piriformis syndrome. More on this follows in part 3.
Piriformis Syndrome
Piriformis syndrome is a neuromuscular condition in which the piriformis muscle irritates or compresses the sciatic nerve. This can lead to radiating pain down the back of the thigh, often mistakenly interpreted as sciatica caused by nerve root involvement in the spine.
Typical symptoms:
• Deep, aching pain in the buttock
• Worsening with sitting, walking, or hip flexion
• Radiation along the course of the sciatic nerve, often not below the knee
• Tenderness over the greater sciatic foramen
• Positive FAIR test, flexion, adduction, internal rotation
The syndrome often occurs as a result of:
• Tight or overactive piriformis
• Weak gluteal musculature
• Dysfunction in the pelvis or lower back
• Excessive repetitive loading, such as running, cycling, or rotational activity
Anatomical Variations and Risk Factors
In most people, the sciatic nerve passes below piriformis, but in 10–15 percent of the population, part or all of the nerve may pass through the muscle. This increases the risk of compression⁴. Other risk factors include:
• Prolonged sitting
• Poor posture and reduced pelvic control
• Trauma or scar tissue around the gluteal region
Clinical Examination
Palpation
• Indirect palpation through gluteus maximus, just over the greater sciatic foramen
• Reproduction of pain is common in piriformis syndrome
Special tests
FAIR test
• Purpose: To reproduce pain related to piriformis syndrome
• Procedure: The patient lies on the side with the affected leg on top, the hip flexed approximately 60–90 degrees, and adduction and internal rotation are performed
• Interpretation: The test is positive if it causes pain or radiation into the buttock or posterior thigh
• Evidence: Often used in clinical practice, but has moderate specificity and sensitivity
Piriformis stretch test
• The patient lies on the back with the affected leg crossed over the opposite knee, with the hip and knee flexed
• Downward pressure on the knee provokes stretch pain in the buttock
Treatment and Physiotherapy
Treatment strategies vary depending on the cause and severity, but the main goals are to reduce muscle tension, improve gluteal activation, and restore normal mobility and strength balance.
1. Manual treatment and stretching techniques
• Stretching of piriformis in flexion and adduction, either lying or sitting
• Trigger point treatment
• Mobilization of the sacroiliac joint when pelvic asymmetry is present
2. Exercises
• Relaxation and control exercises for the gluteal musculature, especially gluteus medius and minimus
• Progression to strengthening exercises for hip extensors and stabilizers
• Dynamic control in the rotational plane, for example standing rotation exercises
3. Neuromotor training
• Focus on the hip–knee–foot chain during functional activities
• Walking and stair training with emphasis on symmetry and control
4. Different modalities
• TENS for pain relief
• Ultrasound or heat as a supplement in acute spasm
Differential Diagnoses
It is important to distinguish piriformis syndrome from:
• Lumbar radiculopathy, with reduced strength, sensation, or reflexes
• Proximal hamstring tendon irritation
• Gluteal bursitis
• Greater trochanteric tendinopathy
MRI or ultrasound is rarely used for diagnosis, but may be useful when structural causes are suspected.
Exercises for Piriformis
Background and Clinical Relevance
Piriformis plays an important role in stabilization of the hip joint and in external rotation of the femur, especially during movements such as walking, rotation, and rising. When function is reduced, such as in piriformis syndrome, increased piriformis activity has been documented as compensation for weakness in gluteus medius and minimus¹. This can lead to compression of the sciatic nerve, reduced hip stability, and pain in the buttock and lower extremity².
Several EMG studies have investigated muscular activation of piriformis during different exercises. There is also support in the literature for the use of stretching and neuromuscular control as part of treatment³.
1. Stretching of Piriformis
Supine piriformis stretch, “figure 4 stretch”
• Research: A study from 2010 showed significantly increased hip joint mobility after 6 weeks of daily piriformis stretching in patients with non-radicular buttock pain⁴.
• Clinical use: Effective for reducing tone and irritation around the sciatic nerve in piriformis syndrome.
• Dosage: 30 seconds x 3, 1–2 times daily.
Seated modified stretch
• Often used in the clinic for patients with reduced mobility. Studies have found that both seated and supine variations increase hip abduction and external rotation without provoking symptoms⁵.
2. Movement Control and Stability
Clamshell with miniband
• Research: EMG studies have shown low to moderate activation of piriformis, 20–30 percent MVIC, and high activation of gluteus medius, 60–80 percent⁶.
• Clinical significance: Improves hip stability and reduces overcompensation in piriformis when gluteus medius is weak.
• Dosage: 12–15 repetitions x 2–3 sets, 3 times per week.
90/90 hip mobility drill
• Recommended in more recent clinical guidelines as part of neuromuscular control and rotational mobility for the hip⁷.
• Increases tolerance for movement and improves joint positioning during internal and external rotation.
3. Activation and Selective Strengthening
Standing external rotation with resistance band, piriformis-specific
• Research: A study published in the Journal of Orthopaedic & Sports Physical Therapy (JOSPT, 2016) showed that standing external rotation with a resistance band provides targeted activation of piriformis, 35–40 percent MVIC, while simultaneously placing low stress on surrounding structures⁸.
• Clinical value: Suitable in the later phase of rehabilitation to regain function without provoking the sciatic nerve.
Single-leg glute bridge
• Research: Although the primary activation occurs in gluteus maximus, piriformis has also been shown to activate as a synergistic rotator and hip extensor⁹.
• Clinical significance: Improves hip control in the lumbopelvic chain and is useful in the transition to functional strength.
4. Evidence-Based Approach to Piriformis Syndrome
According to a systematic review by Boyajian-O’Neill et al. in American Family Physician (2008), treatment of piriformis syndrome should include:
• Stretching, to reduce muscular irritation and compression
• Strengthening exercises, to restore balance in the hip musculature
• Neuromuscular training, to improve movement patterns and reduce overuse
A more recent review by Probst et al. (2020) also highlights that piriformis easily becomes overactive as compensation, and that an appropriate rehabilitation program must include a focus on gluteal function and movement control¹⁰.
Summary
Piriformis should not be trained in isolation for strength alone, but rather as part of a comprehensive hip and pelvic rehabilitation program. Evidence supports:
• Stretching for symptom relief and mobility
• Selective activation using external rotation and control exercises
• Inclusion of gluteus medius and minimus strengthening for unloading
• Gradual exposure to functional loading, such as stairs, walking, and rotation
Sources
Frank H. Netter MD: Atlas of Human Anatomy, 5th Edition, Elsevier Saunders.
Chummy S. Sinnatamby: Last’s Anatomy Regional and Applied, 12th Edition, Churchill Livingstone Elsevier.
Richard L. Drake, A. Wayne Vogl, Adam W. M. Mitchell: Gray’s Anatomy for Students, 2nd Edition, Churchill Livingstone Elsevier.
Jeremy J. MD: Piriformis. Radiopaedia.org, accessed 15/02/2016.
Dissector Answers – Pelvic Neurovasculature. The University of Michigan, accessed 15/02/2016.
Swenson R. DC, MD, PhD: The gluteal region. O'Rahilly 2008, accessed 15/02/2016.